Lowell uses FirstWatch technology and outreach to try and turn tide of overdoses
FirstWatch can help your team track suspected Opioid ODs and Narcan administration, click here to to learn more about leveraging your opioid remediation monies.
Opioid Tracking: Using EMS Data for Suspected Opioid ODs and Narcan Use
Emergency Medical Service (EMS) data has been successfully employed in the past to complement opioid overdose surveillance data provided by the traditional routes. While EMS data still has the limitation of being non-standardized and dependent on the documentation of the EMS provider; it has the advantage of providing information on non-fatal overdoses that would and could not be captured elsewhere. While EMS data in reality starts from a 911 dispatch with a Computer Aided Dispatch (CAD) and in many communities, a call taking set of protocols and guidelines using ProQA or other Emergency Medical Dispatch (EMD) system, moving to an Electronic Patient Care Record (ePCR) rarely are able to trace the entire path that a single 911 call generates within data sources (Diagram 1). Correctly identifying an Opioid Overdose continues to be a challenging task. Its clinical features are non-specific and EMS providers can easily be deceived on the true underlying cause of the present illness. Identifying a set of indicators of overdose that provide key elements throughout the entire EMS data sources can provide a more robust understanding of opioid overdose surveillance within the EMS context.
Diagram 1: Emergency Medical Services (EMS) Data sources.
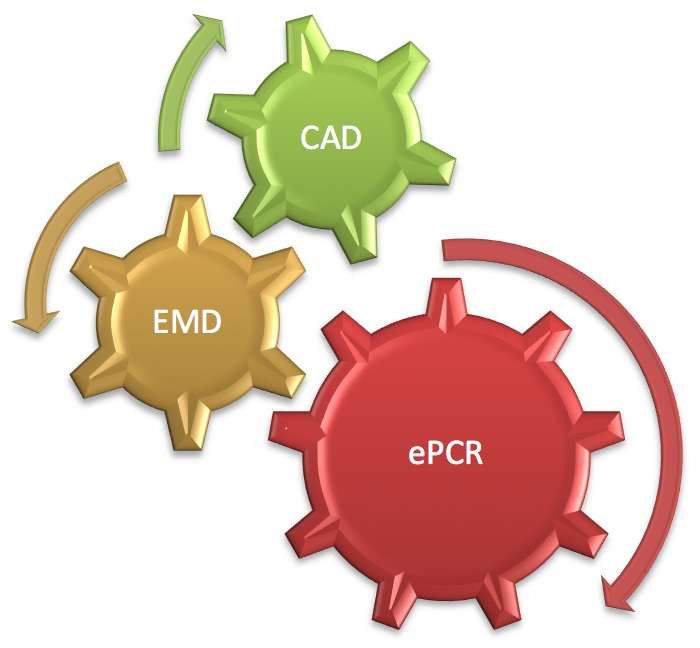
As EMS data is noted to be a typically “dirty” data source of information, in order to mine it for overdose data, one must look in non-standard locations. With that in mind, we have created a set of clinical indicators of overdose that illustrate the acknowledgement of key Data Elements through the entire EMS data (Diagram 2).
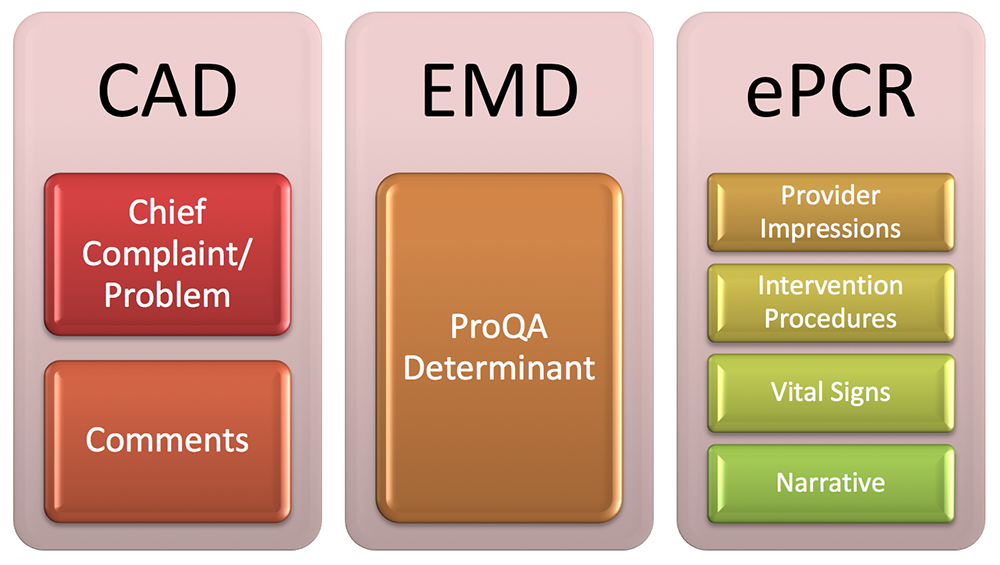
From the above described Data Elements, we have extracted from the CAD system a Chief Complaint or Problem of Overdose/Poisoning ingestion, along with a free text search in the comment section for overdose related keywords. To complement the CAD information, from the EMD we used a ProQA determinant of Protocol 23: Overdose/Poisoning (Ingestion). From the ePCR we obtained a Primary and Secondary Impression of Overdose along with a free text search in the Narrative for any opioid overdose related keyword. We used the identical set of keywords in both the CAD-Comments and ePCR-Narrative free text search (Table 1). An intervention of Narcan/Naloxone administration as well as vital signs where included. From the vital signs we used an altered mental status determined by a Glasgow Coma Score (GCS) of less than or equal to 13 and a decreased Respiratory Rate (RR) rated of less than or equal to 12 per minute.
Diagram 2: Data Elements to identify Opioid Overdose Calls within EMS Data sources
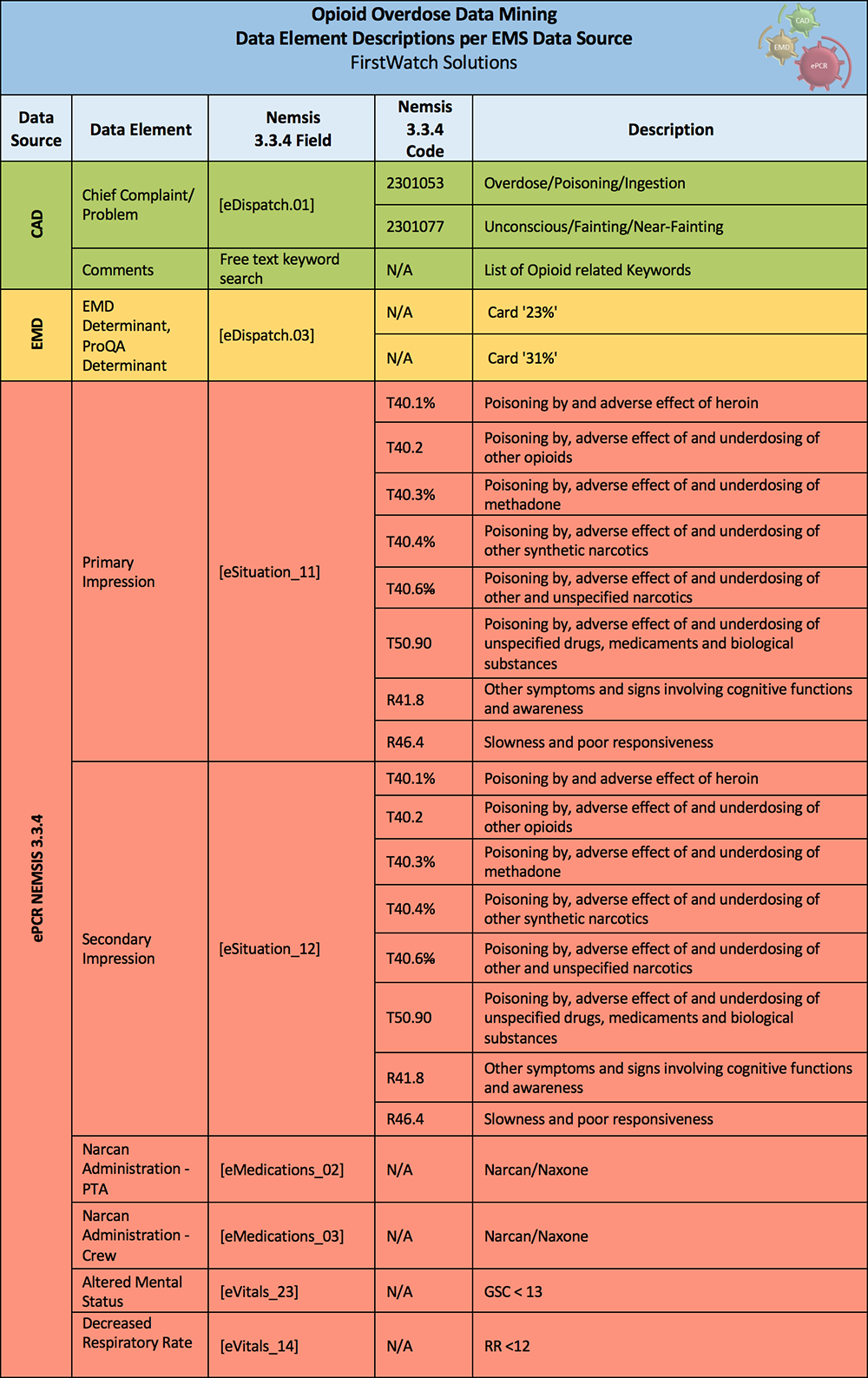
Table 1: Category of Keyword used in Free Text Search for CAD and ePCR.
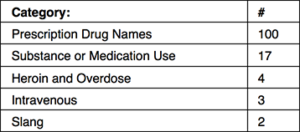
Download spreadsheet “Keyword List for Opioid” for list of keywords, referencing Table 1.
Updated February 15, 2023
Download pdf “Recommendations for Surveillance of EMS Data for Opioid Overdoses” for a duplicate of the above information.
Updated April 10, 2019
Watch the Webinar
View this ISDS Webinar to see how the project got started and to learn more.
Recommendations for Surveillance of EMS Data for Opioid Overdoses
View the Poster
We participated in the International Society for Disease Surveillance (ISDS) Conference, January 29th – February 1st, 2019, in San Diego, California where we presented our findings. Click here for current poster.
Sign up for Notifications on updates to this page and other Public Safety specific Health Intelligence
Please check back with us on this page, or you may alternatively sign up for our Health Intelligence updates and be notified when the recommendations, keyword list, and/or poster have been updated. You may visit our Health Intelligence page for further resources related to awareness and mitigation of opioids and overdoses in response to this nationwide but often local crisis. Click here to sign up.
FirstWatch and Opioid Surveillance
FirstWatch, a longtime partner with public health in general, and specifically with the International Society for Disease Surveillance (ISDS), has focused for 20 years on emergency medical services (EMS) data surveillance for public health and other purposes. EMS data (call taking, dispatch, electronic patient care records) is rich in information, but notoriously non-standardized. FirstWatch monitors for overdoses (of all kinds) for over 200 communities, over half of which are specifically for opioid overdoses. These recommendations are presented to share our evolving experience in this area for the public good. These recommendations are provided as an informative starting point for anyone who wants to monitor their EMS data for opioid overdoses, and are provided as is, with no intended guarantee because every EMS system is different. However, we think and hope that you will find these recommendations helpful and will share your own suggestions here. We will be updating pertinent information on this page, including the Keyword List as we learn more, so we can all make improvements and share best practices for mining EMS data to identify opioid overdoses. If you have suggestions for this page, please contact Jenny Abercrombie, our Marketing Coordinator, at jabercrombie@firstwatch.net.
View this ISDS Webinar to see how the project got started and to learn more.
Recommendations for Surveillance of EMS Data for Opioid Overdoses





